Deep Vein Thrombosis (DVT)
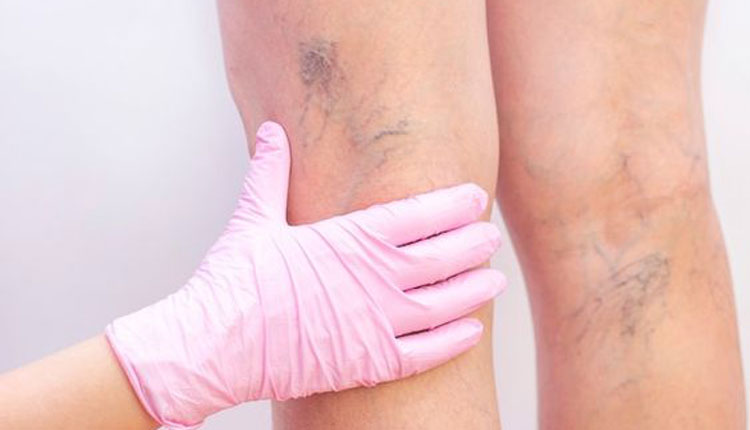
Deep vein thrombosis (DVT, also called venous thrombosis) is a blood clot that develops in a vein deep in the body. The clot may partially or completely block blood flow through the vein. Most DVTs occur in the lower leg, thigh or pelvis, although they also can occur in other parts of the body including the arm, brain, intestines, liver or kidney.
What is the difference between DVT and a superficial venous thrombosis?
A superficial venous thrombosis (also called phlebitis or superficial thrombophlebitis) is a blood clot that develops in a vein close to the surface of the skin. These types of blood clots do not usually travel to the lungs unless they move from the superficial system into the deep venous system first.
What are the symptoms of DVT?
DVT most commonly occurs in just one leg or one arm. Not everyone with DVT will experience symptoms, although when present, they may include:
• Swelling of the leg or arm (sometimes it occurs suddenly)
• Pain or tenderness in the leg that may only be present when standing or walking
• Feeling of increased warmth in the area of the leg or arm that is swollen or that hurts
• Redness or discoloration of the skin
• Enlargement of the superficial veins in the affected leg or arm
What is the acute danger of DVT?
Even though DVT itself is not life-threatening, the blood clot has the potential to break free and travel through the bloodstream, where it can become lodged in the blood vessels of the lung (known as a pulmonary embolism). This can be a life- threatening condition. Therefore, prompt diagnosis and treatment are necessary.
Symptoms of a pulmonary embolism include:
• (Sudden) shortness of breath
• Sharp chest pain, often aggravated by coughing or movement
• Pain in the back
• Cough with or without bloody sputum
• Excessive sweating
• Rapid pulse or breathing
• Lightheadedness or passing out
Some people only find out they have DVT after the clot has moved from the leg or arm and traveled to the lung.
It is important to notify your doctor immediately or go to the emergency room if you have symptoms of a pulmonary embolism or DVT. Do not wait to see if the symptoms will “go away.” Get treatment right away to prevent serious complications.
What is the late complication of DVT ?
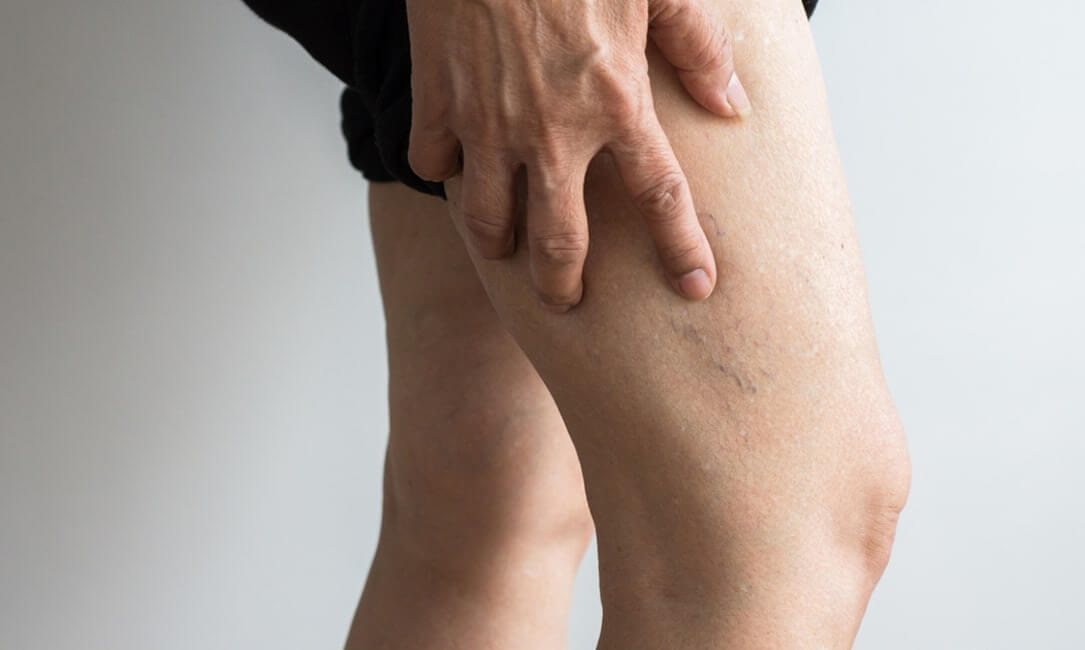
DVT can also lead to complications in the legs referred to as chronic venous insufficiency or the post-thrombotic syndrome. This condition is characterized by pooling of blood, chronic leg swelling, increased pressure, increased pigmentation or discoloration of the skin, and leg ulcers known as venous stasis ulcers.
How is DVT diagnosed?
A duplex venous ultrasound is the most common test used to diagnose deep vein clots. It is used to evaluate the blood flow in the veins and to detect the presence and specific location of blood clots.
How is DVT treated?
Depending on your condition, you may be admitted to the hospital for DVT treatment, or you may receive treatment on an outpatient basis.
Treatments include medications, compression stockings and walking, elevation of the affected leg at rest, and if the blood clot is extensive, more invasive diagnostic and treatment procedures.
Medications
There are several medications used to treat and/or prevent DVT:
Anticoagulants decrease your blood’s ability to clot. Anticoagulants can either come as a pill, such as warfarin (Coumadin) or as an injection or shot, such as heparin or enoxaparin.
Pregnant women cannot take warfarin and will be treated with heparin or low molecular weight heparin only.
Treatment for DVT with anticoagulants usually lasts for at least 3 to 6 months. The following situations may change the length of treatment:
• If your blood clot occurred after a short-term risk like surgery or trauma, your treatment with anticoagulants may be shorter
• If you have had clots before, you may need longer treatment
• If you are being treated for another illness (such as cancer), you may need to take an anticoagulant as long as the risk factor is present
The most common side effect of anticoagulants is bleeding. You should call your doctor right away if you are taking warfarin, heparin, low molecular weight heparin, or fondaparinux and experience easy bruising or bleeding.
Thrombolytics are medications given to quickly dissolve the blood clot. These medications are delivered through a catheter that is directed into the area of the clot. They are used to treat large clots causing severe symptoms.
Compression Stockings
Your doctor should prescribe graduated compression stockings or bandage to reduce the chronic swelling that can occur in the leg after a blood clot has developed and you may need to use it for 2 years.
Medication Guidelines
Take your medications exactly as prescribed and at the same time every day.
Have blood tests as directed by your doctor and keep all scheduled laboratory appointments so your response to the medication can be monitored. Blood tests will evaluate how well your medicine is working. a blood test called PT/INR measures how fast or slow your blood clots. Your medications may be changed or adjusted based on the results of this test.
Talk to your doctor before taking any other medications, especially over-the-counter medications.
Talk to your doctor about your diet, because certain foods affect how well your anticoagulant medication works.
Activity Guidelines
Once DVT occurs, getting around may become more difficult at first,but walking is advised for many reasons after wearing compression bandage or stockings unless your doctor advised against . You should gradually return to your normal activities. If your legs feel swollen or heavy, elevations of legs while at rest will help improve circulation and decrease your leg swelling.
In addition:
• Exercise your lower leg muscles if you are sitting still for long periods of time.
• Stand up and walk for a few minutes every hour while awake.
• Don’t wear tight-fitting clothing that could decrease the circulation in your legs.
________________________________________
If you need more information or would like to make an appointment with a specialist, contact us.
The Treatment of DVT Long-term Side-Effects (Swelling and Painful Leg)
After the initial medical interventions, the most important measurement for preventing and treating of DVD side-effects is to wear the
compression socks (Class 2) for two years, all day long.
If a blood clot is in the veins of the leg, wearing the compression socks below the knee will be enough. But if it is in the veins of thigh, the long
compression socks should be worn.
Usually after the initial medical treatment, the patient is told to hike daily besides wearing the compression socks.
Mostly the status of the patient`s leg will be improved by observing both the mentioned points and the drugs instructions.
Despite all this, the leg may gradually become swelling and painful at the bottom of the leg, around the ankles, the thin skin may also become
discolored and even scarring for some patients.
This situation is called the syndrome after clot or PTS.
PTS treatment is actually the opening of the blood clots in the veins by the use of balloon and stent; fortunately, this treatment is done by
Doctor Aqdasi in Iran since 2011; it has had a very good results.
This patient has been treated by ILIAC STENTING; the right photo shows him after three weeks.
Can DVT be prevented?
If you have never had a deep vein clot, but have an increased risk for developing one, be sure to:
• Exercise your lower leg muscles if you will be sitting still for long periods of time. Stand up and walk regularly. Or get out of the car some times if you are on a long road trip.
• If you are on a long distance flight (more than 4 hours)you must drink a lot (the best is water) , wear loose clothes ,exercise your leg muscles frequently , stand up and walk around at least every hour specially if you are traveling in economy class seat ,and if you are at increased risk then your doctor may prescribe to inject a dose of enoxaparin .
• Get out of bed and move around as soon as you are able after surgery or being ill as directed by your doctor. The sooner you move around, the less chance you have to develop a clot.
• Take medications or use intermittent compression garments to prevent clots after some types of surgery, as directed by your doctor.
• Follow-up with your doctor as recommended to evaluate your risk and follow your doctor’s recommendations for reducing your risk.
If you have had DVT, then you will need to prevent further clots from developing by:
• Taking your medications to prevent or treat blood clots as prescribed by your doctor.
• Keeping your follow-up appointments with your doctor and the laboratory so your response to medications and other treatments can be evaluated.
This essay is translated by Mojgan Salmani